Fibrolamellar carcinoma – causes, side effects and treatments at NaturalPedia.com
Friday, March 23, 2018 by Ralph Flores
http://www.naturalpedia.com/fibrolamellar-carcinoma-causes-side-effects-and-treatments-at-naturalpedia-com.html
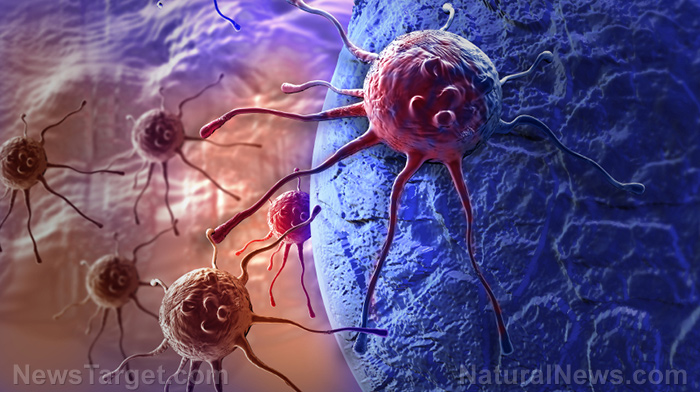
Fibrolamellar carcinoma (FLC) is a rare type of cancer that affects the liver. It is usually seen in adolescents and young adults (before the age of 40). Early stages of FLC are asymptomatic, but later stages may find a person experiencing abdominal pain, weight loss, and malaise – which can be confused with other more common conditions.
Unlike other forms of liver cancer, which is associated with inflammation, viral infections like hepatitis B or C, or alcoholic liver disease and nonalcoholic fatty liver disease (NAFLD), the exact etiology of FLC is unclear, and it can appear even in the absence of inflammation or scarring.
Some studies have related FLC with focal nodular hyperplasia, a benign liver lesion that can found in younger patients, but this has yet to be proven and is still not widely accepted.
In the U.S., the incidence rate of FLC is less than 0.02 in 100,000 people per year, which is even lower than the incidence rate of hepatocellular carcinoma – the primary form of liver cancer – that has an incidence rate of 1.99 per 100,000 per year. Based on case studies, men are three times more likely to get FLC than women.
Known risk factors and symptoms of fibrolamellar carcinoma
While FLC does not have any noticeable symptoms in its early stages, it will develop the following symptoms:
- Pain in the abdomen
- Unexplained weight loss
- General feeling of malaise
In rare cases, the following signs may be present as well:
- Migratory thrombophlebitis (Trousseau syndrome) or a blood clot in the veins, a result of the cancerous mass affecting the inferior vena cava
- Pain and fever that resembles an abscess in the liver
- Obstructive jaundice because of the compression of the bile ducts
- Gynecomastia, that is, the swelling of the breast tissue in men, an effect of the resultant conversion of androgens to estrogens because of FLC.
Other types of liver cancer have hallmark symptoms of chronic disease, a condition which is absent in FLC. For patients with FLC, however, the most common physical sign is the presence of an abdominal mass or fullness.
Body systems affected by fibrolamellar carcinoma
The primary organ affected by FLC is the liver. However, for unresectable (one that cannot be entirely excised) cases, a person’s survival period can be as little as 14 months.
Food items or nutrients that may prevent or relieve fibrolamellar carcinoma
A person’s chances of getting FLC, and even other types of liver cancers, can be mitigated by a healthy diet. Avoiding excessive consumption of alcohol is a key factor in avoiding cancers of the liver. In addition, food items such as broccoli, cranberries, lemons, amla, walnuts, and pecans may aid in the fight against liver cancer, as well as eating foods that are high in phytates like beans, nuts, and grains. Moreover, avoiding added sugars – especially those that contain high fructose corn syrup and table sugar – greatly benefits the liver as these lead to fat buildup.
Treatment and management options for fibrolamellar carcinoma
Resection is the common treatment option for FLC, with a five-year survival rate of 76 percent – higher than that of primary liver cancer that only has a five-year survival rate between 37 to 56 percent at best.
Where to learn more
Summary
Fibrolamellar carcinoma is a rare type of cancer that affects the liver. Early stages of FLC are asymptomatic, but later stages may find a person experiencing abdominal pain, weight loss, and malaise – which can be confused with other more common conditions. Unlike other forms of liver cancer, the exact etiology of FLC is unclear, and it can appear even in the absence of inflammation or scarring.
Resection is the standard treatment option for FLC, with a five-year survival rate of 76 percent. For unresectable cases, however, a person’s survival period can be as little as 14 months.
Sources include:
Tagged Under: Tags: fibrolamellar carcinoma





