Dysphagia – causes, side effects and treatments at NaturalPedia.com
Saturday, March 10, 2018 by Zoey Sky
http://www.naturalpedia.com/dysphagia-causes-side-effects-and-treatments-at-naturalpedia-com.html
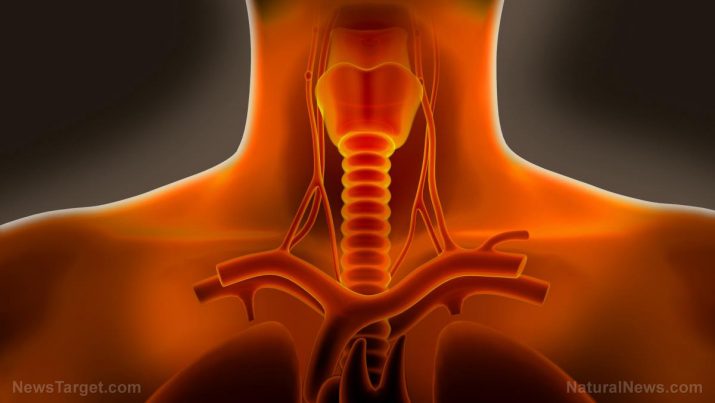
Dysphagia occurs when a person has difficulty swallowing. Some people may also even experience pain while swallowing or odynophagia.
In extreme cases of dysphagia, individuals may be unable to swallow, or they may have difficulty swallowing liquids, foods, or saliva. When this happens, eating can be a challenge.
A person with dysphagia will find it hard to consume enough calories and fluids to keep the body nourished. This may cause additional serious medical problems.
Dysphagia will occur when “there is a problem with the neural control or the structures involved in any part of the swallowing process.” A patient with a weak tongue or cheek muscles may have a hard time moving food around in their mouth while chewing.
A stroke or a different nervous system disorder may make it difficult to initiate the swallowing response, a stimulus that is required so food and liquids can move safely through the throat. Another difficulty can occur when weak throat muscles, e.g. post-cancer surgery, is unable to move all of the food toward the stomach. Dysphagia can also be caused by disorders of the esophagus.
Known side effects of dysphagia
Not all patients are aware that they have dysphagia. If this is the case, the symptom may go undiagnosed and untreated, which can increase the risk for aspiration pneumonia, a lung infection that may develop once saliva or food particles is accidentally inhaled.
The known side effects of dysphagia include:
- Choking when eating
- Coughing/gagging when swallowing
- Difficulty controlling food in the mouth
- Difficulty starting the swallowing process
- Drooling
- The feeling that food is stuck in the throat or chest, or behind the breastbone
- Food or stomach acid backing up into the throat
- Hoarseness
- Inability to control saliva in the mouth
- Recurrent heartburn
- Recurrent pneumonia
- Regurgitation/bringing food back up
- Unexplained weight loss
Risk factors for dysphagia include:
- Aging — Older adults are more at risk because of the general wear and tear on the body as time passes by. Some diseases of old age may cause dysphagia, like Parkinson’s disease.
- Neurological conditions — Some nervous system disorders may increase the risk for dysphagia.
Body systems harmed by dysphagia
Complications of dysphagia include pneumonia and upper respiratory infections, specifically aspiration pneumonia. Other complications include:
- Dehydration — A patient with dysphagia may be unable to drink properly. If their fluid intake is insufficient, they may suffer from dehydration.
- Malnutrition — A patient is often malnourished if they are unaware that they have dysphagia and are not being treated for it. They may not be getting enough vital nutrients to stay healthy.
Food items or nutrients that may prevent dysphagia
Patients with dysphagia may benefit from a level three national dysphagia diet. A level three national dysphagia diet includes moist foods in bite-size pieces, which are easier to chew and swallow.
This diet doesn’t include foods that are hard, sticky, crunchy, or very dry.
Thin liquids may be thickened if they are hard to swallow. The level of thickness a patient needs may depend on their swallowing issues. Consult a healthcare provider to find out how long you have to follow this diet.
To make thickened liquids, use cornstarch, flour, potato flakes, or special thickeners to thin liquids. Thin liquids include:
- Coffee
- Juice
- Milk
- Nutritional supplements
- Soda
- Tea
Foods that are liquid at room temperature must also be thickened. These include:
- Eggnog
- Frozen malts
- Gelatin
- Ice cream
- Milkshakes
- Yogurt
Consult a healthcare professional to find out if you need any of the following types of thickened liquids:
- Nectar-like liquids — These liquids have the same thickness as milkshakes, nectars, and vegetable juices.
- Honey-like liquids — These are thicker than nectar-like liquids. The thickness is similar to honey at room temperature.
- Spoon-thick liquids — These are the thickest liquids. The thickness is similar to that of pudding. These liquids are eaten with a spoon.
When preparing foods for this diet, moisten foods and add flavor using gravies or sauces. Let the food soften before you eat it.
Cook vegetables until they are tender. You can prepare food ahead of time, then freeze it. Reheat the food before you eat it, but don’t let a tough outer crust to form on the food because it might be hard to swallow.
When following a level three national dysphagia diet, you are allowed to eat the following foods:
- Dairy products — Custard, cottage cheese, and pudding. Ice cream, frozen yogurt, malts, and sherbet.
- Grains — Cakes or cookies moistened and softened with milk, coffee, or other liquids. Dry cereals moistened and softened with milk or cooked cereals. Breads, Danish pastries, French toast with syrup or sauce, soft pancakes, and sweet rolls. Soft dumplings moistened with butter or gravy. Rice or wild rice.
- Meat and other protein foods — Casseroles with small chunks of meat, ground meats, or tender meats. Eggs and moistened ground or tender cooked meat, poultry, and fish with gravy or sauce. Strained corn and clam chowder.
- Vegetables and fruits — Baked, boiled, cooked, or mashed potatoes. Canned or cooked fruits without seeds or skins. Cooked and tender vegetables. Shredded lettuce. Soft and peeled fresh fruits such as cantaloupe, honeydew melon, kiwi, mangoes, nectarines, peaches, and watermelon.
Treatments, management plans for dysphagia
Treatment will depend on the type of dysphagia that a patient has: oropharyngeal (caused by a problem in the mouth or pharynx) or oropharyngeal dysphagia.
Since oropharyngeal dysphagia is often a neurological problem, determining which treatment is effective can be challenging. Patients with Parkinson’s disease may respond well to Parkinson’s disease medication.
- Diet — Some foods, liquids, or a combination of them, are easier to swallow. A patient still has to follow a well-balanced diet.
- Feeding through a tube — If the patient is at risk of pneumonia, malnutrition, or dehydration, they may have to be fed through a nasal/nasogastric tube or percutaneous endoscopic gastrostomy (PEG). PEG tubes are surgically implanted directly into the stomach and they pass through a small incision in the abdomen.
- Swallowing therapy — Can be done with a speech and language therapist who will teach the patient new ways of swallowing properly. Exercises can help improve the muscles and how they respond.
Surgical intervention is often required for esophageal dysphagia:
- Botulinum toxin/Botox — This is often used if the muscles in the esophagus have become stiff (achalasia). Botulinum toxin,a strong toxin that can paralyze the stiff muscle, helps reduce constriction.
- Dilation — If the esophagus has to be widened, e.g. because of a stricture, a small balloon may be inserted and then inflated. The balloon will then be removed.
- Surgery — If the dysphagia is caused by cancer, the patient will be referred to an oncologist for treatment. Surgery may be required to remove the tumor.
Where to learn more
- Doctor: Hillary Clinton may have Parkinson’s disease
- Flu shot hoax admitted: “No controlled trials demonstrating a decrease in influenza“
- Hyperbaric oxygen therapy cures woman of stage-4 cancer
- Medical marijuana reduces chronic pharmaceutical use, study finds
- Seven Steps to Gorgeous, Radiant Skin
Summary
Dysphagia occurs when a person has difficulty swallowing. Some people may also even experience pain while swallowing or odynophagia.
Not all patients are aware that they have dysphagia. If this is the case, the symptom may go undiagnosed and untreated, which can increase the risk for aspiration pneumonia, a lung infection that may develop once saliva or food particles is accidentally inhaled.
Risk factors for dysphagia include aging and neurological conditions.
Complications of dysphagia include pneumonia and upper respiratory infections, specifically aspiration pneumonia. Other complications include dehydration and malnutrition.
Patients with dysphagia may benefit from a level three national dysphagia diet. A level three national dysphagia diet includes moist foods in bite-size pieces, which are easier to chew and swallow. This diet doesn’t include foods that are hard, sticky, crunchy, or very dry.
Thin liquids may be thickened if they are hard to swallow. The level of thickness a patient needs may depend on their swallowing issues. Consult a healthcare provider to find out how long you have to follow this diet.
Treatment will depend on the type of dysphagia that a patient has: oropharyngeal (caused by a problem in the mouth or pharynx) or oropharyngeal dysphagia.
Treatment for oropharyngeal dysphagia includes a diet of food that’s easy to swallow, feeding through a trube, or swalllowing therapy.
Surgical intervention is often required for esophageal dysphagia.
Sources include
Tagged Under: Tags: dysphagia





